- Alcohol use disorder (AUD)
- Development and causes of AUD
- Risk factors for developing AUD
- Effects of alcohol withdrawal
- MAT alcohol detox
- How dual diagnosis helps AUD
- The importance of social support in AUD recovery
- Dangers of alcohol as compared to other drugs
- AUD and decision making
- Why alcohol becomes addictive
- Alcohol consumption and AUD in the United States
Alcohol Use Disorder; Everything You Need To Know
Alcohol use disorder (AUD) is sometimes called alcohol addiction, alcohol dependence or alcoholism. It is a common, chronic condition, diagnosed by a healthcare professional and is characterized by excess drinking that causes significant problems in a person’s life. This may have a trickle-down effect and start to affect the lives of those they love. Some people may even find relationships, physical health, careers and other notable parts of their lives are becoming dysfunctional and difficult to manage as a result of AUD.
It is important to remember that addiction arises from patterns of long-term abuse of alcohol and does not happen overnight. Alcohol is one of the most commonly used substances in the United States today. Alcohol use disorder, which should be taken very seriously, benefits from an integrated approach to treatment. People with addictions are often fighting another mental disorder, loneliness, shame and fear. There are many evidence-based treatment programs available to people struggling with AUD, including detox, medically assisted treatment (MAT), social support networks and a whole host of therapies. Although AUD can’t be “cured”, treatment can help to maintain sobriety and enable the person to live a fulfilling life.
Alcohol dependency and alcohol use disorder are caused by a very complex and individualized combination of risk factors, experiences, thought patterns and learned behaviors. An early way of understanding how AUD develops was the Jellinek curve. Over time, it evolved to view AUD as developing in stages.
Stage 1: Occasional Alcohol Abuse and Binge Drinking
Drinking large amounts of alcohol sporadically (for example, only at social events) is not as harmless as it seems. Binge drinking and experimentation with alcohol can have many consequences. Some of the scarier consequences can be alcohol poisoning, coma or even death. It is also seen as the first step towards developing AUD.
Medline Plus defines binge drinking as 5 or more (for men) and 4 or more (for women) alcoholic drinks within 2 hours. Often binge drinkers far exceed this amount. It is more common in young adulthood, when people have just started to experiment with alcohol. They often want to push their bodies’ limits and may be facing social pressures to attend events that focus on drinking for “fun”. If the person starts to get dependent on the feelings associated with binge drinking and starts to do it more frequently, they may progress to the next stage.
Stage 2: Developing tolerance for alcohol and increased drinking
Stage 2 is when drinking is no longer experimental and increases in frequency (for example, drinking over weekends as well as at social events). The main characteristic of this stage is when the person starts to develop an emotional attachment to drinking. This attachment may be because alcohol use has caused a reduction in anxiety, boredom or stress in addition to suppressing feelings of fear or loneliness. Although increased frequency or quantity of drinking is a concerning and important consideration, the emotional attachment to drinking is often considered the defining characteristic stage 2.
Stage 3: Problem drinking
This stage is characterized by the presence of negative side-effects from uncontrolled drinking habits. The impact of the short- and long-term consequences of drinking begins to make the drinker less functional in their everyday lives.
They may become anxious, depressed, and have poorer quality sleep. Social problems like relationship issues, self-isolation and sudden changes in friends can start to be seen. Physical problems like nausea and headaches start to catch up with the drinker. Despite these and many other possible problems arising in their lives, the person may still drink because they enjoy it.
Stage 4: Alcohol dependence
Although the person may be aware of the negative side-effects of uncontrolled drinking, by this stage they are often physically unable to stop using alcohol. Physical dependence on alcohol has two aspects: tolerance and withdrawal. With chronic alcohol use, the body requires more and more alcohol to get the same effects (tolerance). At this stage, if the person stops using alcohol, they will likely develop a range of physical symptoms that can range from unpleasant to life-threatening (withdrawal). Chemical dependence on alcohol is one of the reasons alcohol use can evolve into addiction.
Stage 5: Alcohol addiction / alcohol use disorder
By this stage the person is physically and psychologically compelled to drink. By now the original factors that made alcohol use seem appealing in stages 1 and 2 may be giving diminishing returns or have increasingly negative consequences, yet the person cannot stop drinking. They may want to, but find themselves going into withdrawal without alcohol or be unable to think about anything but their next drink. Without alcohol they may not be able to function in their everyday life, but understand that their drinking is making it harder and harder to do so. By this stage, a person’s whole life often revolves around alcohol use and the short- and long-term consequences that come with it.
The consequences of alcohol consumption can be devastating, no matter the stage. Treatment is not reserved for people who are in stage 5. If you feel that you or a loved one is using alcohol as a way to cope with other problems or that alcohol use is having a negative impact, treatment is available.
- Quantity, frequency and rate of alcohol consumption
- Genetics (while AUD has about a 60 percent heritability rate, AUD is not exclusively caused by genetics, but the interplay between genetics and psychosocial factors)
- Family history of alcohol abuse
- Adverse childhood experiences (ACEs)
- Social and cultural attitudes to drinking alcohol
- Low socioeconomic status
- Ease of access to alcohol
- Experiencing trauma (such as physical or sexual abuse)
Co-occurring mental illnesses may contribute to, result from or co-exist with AUD. This includes schizophrenia, mood disorders and some personality disorders.
Diagnosis of Alcohol Use Disorder
Alcohol use disorder (AUD) is a diagnosis made by a healthcare provider, based on the Diagnostic and Statistical Manual 5 (DSM-5). This manual lists 11 factors that you should consider when researching if you or a loved one might have AUD.
Some of the 11 Factors Considered are:
How often, in the last 12 months, has a person experienced:
- Drinking more or longer than they thought they would
- Wanting to completely stop or cut down on their drinking, but not being able to
- Wanting a drink so badly that they couldn’t focus on anything else
- Continuing to drink, despite it making them anxious, depressed or adding to health problems
The severity of the disorder can be determined by how many of these factors apply within the last year. It is considered mild alcohol use disorder if the person has had 2-3 of the symptoms listed. Moderate AUD is when the person experiences 4-5 of the factors and a severe AUD diagnosis includes 6 or more. The most important considerations, however, are if they meet 2 or more of these criteria and if alcohol consumption makes a person less able to function in their everyday life. If a healthcare provider diagnoses a person with AUD, they will strongly encourage them to seek treatment. No-one should suffer a chronic illness without treatment, especially when there are so many treatment options for AUD.



Each person’s body reacts differently in withdrawal, but stopping suddenly has a very real risk of death. The severity of the symptoms can range from mild to urgently needing medical attention to avoid life-threatening complications. You may not experience all of them, but no-one knows how severe their alcohol withdrawal will be until it happens. It can be dangerous to quit drinking “cold-turkey” in an unsupervised environment – withdrawal symptoms can be quite severe and made worse by underlying health conditions. It is strongly recommended that you talk to your doctor or an inpatient treatment facility before you quit drinking. An inpatient facility with a detox center, like Lakeview Health’s, will be able to monitor your health and progress and keep you safe from potentially harmful alcohol withdrawal symptoms.
Although each person’s experience of withdrawal will be unique, even medical professionals cannot predict how badly your body may react to suddenly stopping drinking. The above timelines are an estimate and some medical professionals prefer to determine how to help you manage withdrawal symptoms based on their severity, rather than by timeline.
While milder symptoms may be manageable on an outpatient basis, it is always advised to be under the guidance of a medical professional. These risk factors increase the chance of experiencing more severe withdrawal symptoms:
- Poor or no support system
- Abnormal laboratory results (as reviewed by your health professional)
- High risk of experiencing delirium tremens
- Have had withdrawal seizures in the past
- A dual diagnosis Abuses other substances Suicidal ideation or previous attempts at suicide
Knowing these risk factors can ensure that medical help is at hand if symptoms increase in severity. In many cases, they can even help prevent life-threatening symptoms from developing. Alone, you would have none of these tools, clinical experts and scientifically-based support methods. Don’t face a potentially life-threatening process alone, when support is available.
A safe and successful detox is the first step in treatment at a rehabilitation center with a medical detox center, such as Lakeview Health. People may resist seeking treatment, as they fear the detox process, but a medically monitored detox program makes the process as safe and comfortable as possible. Although each facility may differ slightly, detox at a rehabilitation center generally includes:
Medical assessments: As mentioned earlier, many pre-existing medical conditions may increase the risk for dangerous withdrawal symptoms. Intake assessments help the clinicians who will be managing and monitoring the detox process to create an individualized treatment program, accounting for potential risks and complications.
Withdrawal: Under the care of healthcare professionals, the patient will start to experience some of the physical and psychological withdrawal symptoms mentioned above. Typically, alcohol withdrawal symptoms peak at 24 to 72 hours after that last drink, with milder symptoms possibly continuing for a few weeks. Medical detox centers maintain a calm and controlled environment to minimize the withdrawal effects as much as possible.
Medication: Clinical staff manage dangerous withdrawal symptoms around the clock. With 24/7 supervision, clinical staff can also provide medications and treatments to mitigate the risks of the patient developing severe withdrawal symptoms. One such intervention is administering IV rehydration to correct electrolyte imbalances. Another IV mix of nutrients is called a “banana bag”. It contains folate, thiamine, basic sugars and lots of multivitamins, which ensures that the body has the extra nourishment it needs. This mixture works to lower the risk of developing a very serious degenerative brain disorder called Wernicke-Korsakoff Syndrome, which often develops with alcohol abuse.
Medication-assisted treatment (MAT) can also help to reduce the negative effects of withdrawal. Other treatments are more effective when an individual is not constantly battling their cravings and withdrawal symptoms. Psychoeducation on how these medications work and why someone may decide to take them as a part of their recovery will also occur during this period of treatment.
All of these clinical interventions can make withdrawal manageable and much safer. Although post-acute withdrawal syndrome (or PAWS) could persist following detoxification, the first four days of medically monitored detox are the toughest. That’s why it’s vital to be under the watchful, caring eye of medical professionals 24/7. During the entire process, they’ll monitor your physical health and overall stability. They’ll also ensure that you’re not over-medicated, minimizing the potential to develop a secondary addiction.
There is a train of thought that detoxing “cures” the addiction, but it only addresses the physical aspect of treatment. The treatments that follow focus on recovery through understanding the psychological and behavioral aspects of addiction. With a chemically clear body, these aspects of treatment can be explored through therapeutic methods.
Oftentimes, alcohol addiction occurs alongside another mental health disorder. Determining if a person has any co-occurring disorders is crucial in creating a treatment plan. Mental health conditions can significantly complicate an alcohol addiction. Many individuals fail to receive the diagnosis or care they need for their co-occurring mental health disorder, which may lead to returning to alcohol abuse to manage their symptoms.
As of 2019, 9.5 million people (between 18 and 25 years old and living in the US) reported that they had been diagnosed with a mental disorder as well as a substance use disorder. These only include people who have been officially diagnosed, so the number may be even higher. Only 742,000 (7.8 percent) of them had received treatment for their dual diagnosis. The most common mental health disorders to occur alongside AUD are anxiety and mood disorders.
Dual diagnoses may include AUD and:
- Mood disorders
- Depression Bipolar disorder
- Anxiety disorders PTSD
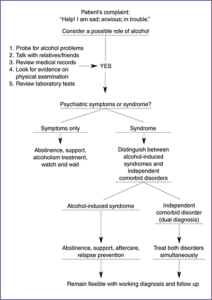
Co-occurring mental disorders may contribute to, co-exist with or be caused by AUD and often share many risk factors. This makes it very difficult to say if one caused the other or if they both occurred independently. To the person living with both of these disorders, the most critical aspect of a dual diagnosis is that they are treated together and that the clinician stays flexible in terms of treatment and diagnosis.
This diagram by Antenelli, made in 1997, shows how a dual diagnosis can be determined by a health professional:
Through dual diagnosis treatment at an alcohol addiction treatment center, such as Lakeview Health, you are able to receive care for both issues at the same time. When you contact the treatment team, we perform a comprehensive evaluation. This evaluation determines whether you are battling an additional mental health condition as well as alcohol use disorder. The intake assessment helps in developing a personalized treatment plan.
Lakeview Health’s dual diagnosis program Offers:
- Medication management
- Mood stabilization and continued monitoring by licensed physicians
- Relapse prevention techniques for addiction
- Education on coping skills for managing mental health disorders
- Resolution of underlying issues contributing to dual diagnosis
Counselling with family or significant others to increase awareness about dual diagnosis
Treatment plans consider co-occurring conditions, such as:
By understanding that these disorders may require their own specific coping strategies and what these might be, you can avoid abusing alcohol to manage their symptoms. This can make a difference to your overall recovery journey and help prevent relapse in the future.
Disorders like AUD often lead to increased shame, fear, isolation and loneliness. Addiction is something no-one should face alone. Social support during your stay at Lakeview Health helps in connecting you with mentors, treatment experts and other people struggling with substance abuse. We treat the individual, but also remind patients that they are not alone.
The True North Alumni program ensures that patients never have to feel isolated in their recovery, even after leaving the treatment facility. In the grand scheme of things, the time in a treatment facility is short in comparison to the full recovery journey. To make the impact of treatment stick – and to navigate the ups and downs of the recovery process – Lakeview Health offers ongoing aftercare support. Support that is available for months and years, not just days and weeks.
Alcohol use has become so normalized that we often don’t even refer to it as a drug. The way drugs are classified may make it seem that illegal drugs, like heroin or cocaine, are deadlier than alcohol. Many people see alcohol as a socially acceptable way to relax and as “safe” to use in moderation. The scientific research says the opposite; alcohol is one of the deadliest drugs of all.
In 2019 the National Survey on Drugs Use and Health reported that 95,000 people die from alcohol related deaths in the US each year. Between 2006 and 2014 there was a 61.6 percent increase in alcohol-related emergency department (ED) deaths, from 3,080,214 to 4,976,136. Each year the average number of emergency department visits related to alcohol increased by about 210,000 cases. This resulted in an increase in costs associated with ED visits from $4.1 billion to $15.3 billion.
According to Vista Research Group’s 2020 report on Lakeview Health, intake records of 1,341 patients from 2019-2020 reported that 57 percent of patients in treatment named alcohol as their drug of choice.
One of the challenges in deciding which drug is the “worst” or most harmful is deciding what “harm” is and how much of it that drug does. A panel of scientists and experts in addiction was formed to answer this question – the Independent Scientific Committee on Drugs (ICSD). They made a scale that measures the harm that different drugs could do to both the individual and society. It ranges from 0 (no harm) to 100 (the most possible harm).
The panel used this figure to show how harm was broken down to evaluate all the ways drugs can cause it. They ended up with 9 ways drugs harm the person and 7 ways they harm society.
Considering damage to both the person and their society, alcohol (scoring 72 out of 100) was the most harmful drug in the study. It caused more overall harm than heroin (55), crack (54), crystal meth (33), cocaine (27) and tobacco (26). If you consider damage to the individual alone, heroin, crack and crystal meth were the most harmful drugs. In terms of damage to society, alcohol, heroin and crack caused the most harm to others. The true extent of alcohol’s dangers can be seen in its many short- and long-term consequences.
Alcohol affects our bodies from the first sip. Alcohol reaches your brain within 30 seconds. The main form of alcohol that people consume is called ethanol. It is a central nervous system (CNS) depressant, which means that it slows down how fast our brains can send messages to the rest of our bodies. Alcohol affects and is processed by many different organs. This results in many of the short and long-term consequences associated with drinking alcohol.
Short-term consequences of alcohol include:
- Altered mood
- Slower reflexes
- Poor balance
- Impaired thought and decision-making
- Impaired ability to store memories
- Poor sleep quality Frequent need to urinate (causing dehydration and headaches)
- Gastrointestinal issues (such as heartburn, nausea, vomiting and/or diarrhea)
Although the short-term effects of alcohol seem to “disappear” the next day, your body is left to deal with more than just a hangover. Frequent binge-drinking and long-term use of alcohol can lead to permanent changes to your body.
Long-term consequences of alcohol include:
- Bad quality of sleep
- Heart disease (such as dilated cardiomyopathy, harmful arrythmias)
- High blood pressure (hypertension)
- Damage to your throat (from constant acid reflux or vomiting)
- Damage to small and large intestines (alcohol changes how food passes through them)
- Kidney damage (frequent urination increases their workload and alcohol itself is a toxin that is constantly passing through them)
- Liver disease (cirrhosis – constantly breaking down the toxins in alcohol causes the buildup of fat and fibrous tissues in the liver. This means that liver cells don’t get enough blood flow and die, leaving scars and damaging your liver)
- Diabetes (alcohol can cause chronic pancreas inflammation, which can result in diabetes) Obesity (many alcoholic beverages have a high caloric value)
- Malnutrition
- Poor body temperature regulation
- Hearing loss
Increased risk of cancer, especially of the:
- Mouth
- Throat
- Voice box
- Esophagus
- Liver
- Pancreas
- Colon and rectum
- Breast
- Stomach
The American Cancer Society explains that, for most alcohol-associated cancers, the more you drink, the higher your risk of developing the disease. However, in some, like breast cancer, a person increases their risk by drinking even small amounts of alcohol. Other cancers associated with alcohol are caused by the over-working of organs and their cells, like the liver and pancreas. Although alcohol damage to organs like the heart, liver and kidneys has dominated the media in the past, alcohol-related damage to your brain is being researched more and more. Long-term alcohol use leads to alterations in the brain’s chemical balance and structure and can have far-reaching consequences. Alcohol affects the brain in ways that could permanently alter how people live their lives.
Long-term Consequences of Alcohol on the Brain Include:
- Decreased brain size (brain cells shrink and change)
- Difficulties in controlling your movements
- Poor balance (damage to the cerebellum)
- Increased risk of stroke
Alcohol-Related Changes to Brain Structure can Lead to Behavioral and Psychological Issues, such as:
- Impaired thinking and poorer decision-making abilities
- Difficulties in storing and retrieving memories
- Dementia (from global brain cell damage and damage to the memory centers of the brain)
- Mood swings Learning difficulties
- Changes to personality (associated with decreased size of the frontal lobe)
- Loss of productivity and motivation
It’s not uncommon for people with alcohol abuse problems to isolate themselves from others in order to hide their drinking habits. Isolation plus the physical and mental issues that come with long-term alcohol use can cause people to feel even more alone. They may drink more as a coping strategy. This self-destructive cycle often develops slowly. Whether short-term or long-term, alcohol can have physical, psychological and social consequences that have a profound influence on decision-making and behavior.
When individuals drink, alcohol begins to interfere with the communication pathways in the brain. This interference can cause mood swings, memory lapses, changes in behavior, loss of co-ordination and hearing, and an inability to think clearly. If people drink enough, they can lose control of these functions entirely. Drinking too much even once can cause people to make poor life choices.
Unintended Outcomes Associated with Alcohol Use may Include:
- Accidental injuries (such as falling or drowning)
- Car or motorcycle accidents
- Violence toward self or others
- Risky physical or sexual actions
- Harmful medication interactions
- Alcohol poisoning
- Damage to important relationships
- Unemployment
- Destitution
- Destructive behaviors that often result in further alcohol use to cope with the negative outcomes
- Emotional distress
- Uncontrollable mood swings
- Death
All of these unintended events can have lasting changes in an individual’s life. Regular alcohol abuse makes the possibility of adverse outcomes more and more likely. Eventually, it’s going to be impossible to avoid some the unforeseen consequences of drinking, no matter how hard someone tries.
Statistics on alcohol consumption in the US were recorded in the 2019 National Survey on Drug Use and Health (NSDUH).
These were some of their findings:
Prevalence of Drinking in the US:
- 85.6 percent of people over 18 years old had consumed alcohol within their lifetime
- Within the past year, 69.5 percent of people over 18 had drunk alcohol
- Within the past month, 55.9 percent of this age group had consumed alcohol
- Binge drinking was reported in 25.8 percent of this age group within the last month
- Heavy alcohol use within the last month was reported by 6.3 percent of over 18s
Prevalence of AUD in the US:
- 14.5 million people over 12 years old (5.3 percent of all the people within that age group) had AUD
- Men: 9 million
- Women: 5.5 million
- Of these, only 7.2 percent had been in a form of treatment within the last year They were more likely to seek medical care for an alcohol-related problem than for AUD
- Only 4% of people with AUD over 12 years old had received medical treatment with prescribed, U.S. Food and Drug Administration (FDA) approved drugs for their disorder.
Although many people in the US drink alcohol, not all of them will become addicted to it. What makes alcohol addictive? Why is alcohol not equally addictive to everyone?
A chemical dependence on alcohol, created over time, is an important reason of why people become addicted. Alcohol is a depressant, which slows down the body and mind. To combat the “downer” effects of chronic alcohol use, the body attempts to balance itself out by “speeding up”, usually using adrenalin and chemical messengers to achieve this. It also learns how to cope with the intoxicating effects of alcohol. This is called tolerance. Over time, more and more alcohol must be consumed to get the same effects. With chronic use, the body will build up a tolerance for alcohol and a dependency on it.
When alcohol is not available, the chronic “speed up” effects that the body uses to combat the depressant effects of alcohol needs time to return to baseline. During this time, our body systems are out of balance and we get a range of physical symptoms called withdrawal. Withdrawal can be a physically harrowing and a potentially life-threatening process. Avoiding withdrawal symptoms by drinking more and more alcohol is often an integral process in the development of AUD.
How our brains react to alcohol is another important factor in determining if someone will become addicted or not. Ethanol (the alcohol used in alcoholic beverages) is a central nervous system depressant. It affects different neurotransmitters (chemical messengers) in the brain because it can cross the blood-brain barrier. This makes it extremely effective at creating changes in various neurotransmitter pathways as well as a damaging toxin. Ethanol affects dopamine, 5-HT, γ-aminobutyric acid, glutamate, endogenous opioid transmitter, acetylcholine and norepinephrine. While each of these play important roles in alcohol addiction, some specific neurotransmitters and how they contribute include:
GABA
One of the main inhibitory neurotransmitters (chemicals) in the brain is GABA (gamma-aminobutyric acid). GABA has special sites where ethanol binds to it and blocks brain signals. This is how alcohol creates the perception of stress and anxiety reduction.
Glutamate
Alcohol also binds to another neurotransmitter called glutamate. Glutamate has an excitatory (activating) effect on the brain. Instead of increasing its excitatory effect though, ethanol decreases it. This enhances the depressive effects of alcohol and might be responsible for the learning and memory problems many chronic alcohol users face.
Dopamine
While many drugs target the dopaminergic pathways in the brain, alcohol does so on multiple levels. The first is by directly activating this pathway, which triggers a reward response and a chemically induced feeling of pleasure that increases as the person drinks more and more. Alcohol can also “hijack” dopaminergic responses indirectly. When engaging in something that potentially brings feelings of joy, social belonging, reduced stress and a “calmer” mind, dopamine (often referred to as the reward and motivation neurotransmitter) is released to encourage doing this behavior (drinking alcohol) again.
Naturally, we all have different levels of these chemicals and some people are more responsive to the effects of ethanol than others. Variability in neurotransmitter response to alcohol is also genetic. Genes that affect how enzymes that metabolize alcohol are encoded and genes that encode neurotransmitters and their receptors (D1, D2 and D4 in particular) are integral in forming an addiction to alcohol. Combined with the potential imbalances in neurotransmitters that some mental illnesses that commonly co-occur with AUD, like anxiety or depression, can cause, it becomes difficult to know exactly how each person will react to and experience alcohol.
In general, these alcohol-related brain changes mean that the brain remembers that consumption was associated with pleasure and that stopping can lead to psychological and physical pain (if alcohol dependence forms). When adding other risk or protective factors to the equation, it becomes obvious that it is very difficult to pin down exactly why some people become addicted and others not. It is not as simple as a “choice” to develop AUD; many of the risk factors for forming an addiction are not the individual’s control.
Our team has experience treating people from a range of backgrounds, giving each person the tools that they need to recover from substance use.
Lakeview Health offers a variety of addiction treatment programs for those struggling with alcohol addiction and provides gender-responsive programs.
Treatment Programs Include:
"*" indicates required fields